Starting in June of 2021, HCVME will be doing quarterly newsletters! on Viral hepatitis, COVID19 pandemic, and Liver transplant related stuff, but it will expand to more public health related things, so keep an eye out! For now it’s mostly an expansion of my blog and articles. Please sign up!
Category: Uncategorized
Hepatitis C You Later 2020
HCVME 2020 Review, Each Year, I’m going to add to this story, little by little, to keep you updated on my journey from diagnosis to transplant to treatment, to helping eliminate Hepatitis C.
It was a hot summer day in late July of 1999; Y2 K was the biggest concern on anyone’s mind, but I was 12, my concerns lay in how much pizza I could get from the pizza party coming up that Friday. I was in Tennis camp, and while I wasn’t great at Tennis, I was great at eating pizza. It was still a few days away, and like most 12-year-olds, I’d drink Gatorade and sodas in between the class sessions. But when my dad picked me up that day, I had little clue about how much all of our lives would change from such a small series of events. Upon arriving home, I rushed to the bathroom. The color was unusual, a dark, iced-tea colored urine; alarmed, I called over my dad. Upon his inspection, we decided a visit to the doctor was in order. After that point, the pizza party seemed a lot further away. When my doctor brought my family in, he wasn’t sure what he was looking at; the blood tests were inconclusive, so he explained a biopsy would help find the culprit. I was twelve, and it was 1999; Biopsy was the standard still, and I was more excited that this Saturday I would get to watch more than my allocated 30 minutes of cartoons. They’d decided to biopsy my liver, spleen, and kidney because they weren’t sure where the internal bleeding came from, and my platelets were fine. Although I had no idea this was happening, I was more focused on the McDonalds at the entrance to the hospital and the potential for Chicken Nuggets.
My follow up appointment in September made all the chicken nuggets, pizza parties, and cartoons seem entirely irrelevant. The doctor explained to my family and me that I had Hepatitis C (HCV), which was unusual for a 12-year-old, so they tested the rest of my family. The doctor also explained that because of how the disease progresses, and that I likely had it since birth and that by 30, I would need a liver transplant or die. I am glad that he was serious in his explanation and that he didn’t hold back any information. At that time, there was no cure for Hep C; there was a sliver of hope, though through a life-altering treatment. When my family’s tests came back, we were relieved when my father and brother tested negative for Hep C. But it had confirmed the doctor’s suspicion that my mom was the source, as we had the same strain of HCV. My mom was devastated, I didn’t understand how to feel. I knew that I was 12 and that I was potentially already at the midpoint in my life, so my goals and dreams faded. While there was no cure in 1999, there was treatment with a less than 30% success rate. The treatment required a year of thrice-weekly injections and a series of pills. Non-PEGylated Interferon and Ribavirin, when she took them, my mom began acting almost bipolar in her characteristics. It was hard to understand what she was going through for any of us. But Interferon essentially makes you feel like your worst flu, a dozen times over, and ribavirin can encourage emotional swings, skin issues, and both enhance fatigue. My mom made it through nearly ten months before the treatment failed her. It took years for my family to recover, but there wasn’t much time for that. She found a new job, and I entered High School. My dad had made an agreement with the school to preempt anything they may do: they would pull me out of all sports and any sports teams, and I would be barred from joining. Which meant leaving Tennis, Swimming, Wrestling, and Basketball behind. I didn’t know to talk to others about my Hep C, so I freely explained my circumstances to everyone I knew. I didn’t know that faculty and parents would react so negatively to something which could affect them in no way except their own misunderstandings and fear.
I was lucky in a way; 2002 happened to be the year a lot more people learned about Hep C. Mostly through gossip and rumors regarding Pamela Anderson and her former relationship with Tommy Lee. She was infected through a tattoo needle, although her status as a sex symbol meant that kids my age assumed it was a Sexually Transmitted Disease/Infection. By then, I realized I should be more selective with whom I share my status. My mom was ramping up for her second treatment, a PEGylated version of what she’d taken before. This version only required one injection per week but still lasted 48 weeks. This treatment would also ultimately fail her, but we still had hope it might work for me. Once I turned 18, I was given the option to take that same treatment, but I wanted to wait for better timing with school because I’d seen the debilitating state the treatment had left my mom. And as the magnet on my fridge reminded me: When you miss school, you miss out. So I waited until my senior year of college while in a long-distance relationship with an unsupportive fiancé. She wanted me to move out to Florida as she’d done nearly a year before, but my decision to treat while living with my family and having friends nearby turned out the be the best decision I could have made. She was resistant and frustrated with my choice, and it was made because I knew what I would go through; I knew the risks. I also knew that when I graduated, I could lose my health insurance, so it wouldn’t be covered otherwise until I got a full-time job. And even then, it would be a preexisting condition, so it became even more complex, and all of this was lost in our arguments. The stress was unreal, and the treatment I thought I’d prepared for was worse than I could have imagined. For three months, between my hormones pushing me to cry at doorknobs and the daily fatigue having me miss work for the first time, I was in pieces. I walked with a cane because my legs were weak from the injection sites; I used a megaphone to speak to the kids I worked with because my voice would go. I tried my best to stay in a doomed relationship, which my treatment’s failure would ultimately help me realize that maybe we weren’t right for each other. When the treatment failed, I was crushed. I didn’t know what to do; my mom was equally devastated, having hoped that maybe it would work for me, that maybe her pain wasn’t pointless.
With the help of my kids in the program I worked at, of my friends that summer, and my family supporting me, I found renewed purpose. I hit the gym, I reinvented myself, and after a few months of exploring my budding identity, I found some peace. Two years later, my doctor would suggest that I try the treatment again, only with a higher dosage. This was an unnecessary treatment. It was a year before the first Direct Acting Antivirals would come out. He was more interested in pushing the treatment because he was working for the company that made it. I learned of this years later thanks to OpenPayments, a searchable database of payments doctors receive. This was the beginning of my life with cirrhosis. Just as you’d imagine, the treatment was a bit worse than my first, and equally devastating when my viral load stayed at 3 million.(Viral load indicates the viral quantity but not the severity of illness, below 500k, is low, 500k-5mil is high, and above 5 mil very high.) I was a wreck, and my behavior and choices reflected my depreciating attitude about life. But I put myself back into again, hit the gym, reinvented myself again, and started running a before/after school care organization.
That next year, my mom would go on the single roughest treatment either of us would take. The regimen called for 3 months with the new DAA, and then 6 months additional without it. It was dubbed the triple cocktail, an ironic name as this was for liver disease. Interferon, Ribavirin, and Incivek would ravage my mom’s body requiring multiple units of blood and Procrit to keep her alive.
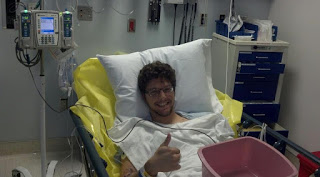
Ultimately she would find that her hell had paid off and was cured on her third treatment. While the Affordable Care Act had recently been passed, its stance was shaky, and I was worried about my preexisting condition preventing me from accessing insurance. And so, in the two months between when I turned 26 and my new tech support job’s insurance kicking in, I opted to fork over half my paycheck for two months of COBRA.( Consolidated Omnibus Budget Reconciliation Act Insurance can be used when employer health insurance ends for an individual, although it’s quite costly since a person pays both the employee and employer share.) Then I prepared for what I hoped would be my last treatment. I worked out for months prior, ate healthier, and tried to make the only factor that poorly affected my health, the virus. My new friend, at the time, who is now an RN, walked with me through the rough of it. My friends helped me deal with the unusual requirements of the treatment. I was to eat 10 grams of fat with each pill, which is rather hard when one has no appetite. So I’d stuff my face with crumb donettes while taking my pills, or a handful of nuts, depending on which was available. The treatment was twice as hard as anything else I’d taken previously, and it would bring me to the floor in exhaustion. I remember using a good deal of FMLA that year, so much so I’d been missed out on multiple promotion opportunities. Family Medical Leave Act allows for up to 12 weeks of unconsecutive unpaid time off. Three months after I’d started my third treatment, I found myself in a hospital ER asking for a puke bucket. Not a few seconds later, however, missing the bucket altogether, but thankfully the floor would catch most of the nearly two units of blood that projected itself from my mouth like a font. The next few moments were a bit hazy, but needless to say, they gave me an express pass to a bed; I skipped the whole ER line. They began the process to infuse blood and figure out where the internal bleeding was coming from. Had I not recognized the signs from a previous hospitalization, I’d probably have bled out even more en route to the hospital and likely died.
This was the beginning of my symptoms regularly manifesting, as prior to treatment, I’d received a MELD score, indicating the need for a liver transplant. A Model for End-stage Liver Disease score is given to patients awaiting liver transplant to show their imminent need for transplantation; the higher the score, the lower chance of living the next six months and the better chance at receiving a transplant. I was creeping closer to thirty, so my diagnosing doc’s warning was ringing in my ears. This failure was hard to accept, but like the others, I reassessed my life. I decided to leave my new job in tech support and return to working with kids. Unfortunately, over the year, I was building up my strength; my liver disease was making up for the treatments I’d been doing. My legs began to swell and retain fluid, an unusual manifestation of ascites; I’d been diagnosed with every symptom which comes with end-stage liver disease.
Hepatic Encephalopathy was the trickiest one, and one who helped get me relieved of the field I’d just reentered. Without daily lactulose, I could get trapped in mental circles mirroring dementia. My inability to do basic math proved challenging, but by using an excel spreadsheet, I felt I could compensate. My new job, however, came with new problems. The problem wasn’t my health; the problem was that I wasn’t who she wanted to hire, so they told me I was the best candidate they’d seen and was welcome to reapply; however, this position was determined to not be a right fit. The entire time I was working, she’d used my health as an excuse to push me out, encouraging me to take sick days during my evaluation period, planning meetings on days where I had appointments, knowing all of this would hurt my chances to become a permanent employee. After being let go, I was beside myself. This was the field I’d learned so well that they would ask me to come back as a consultant to help improve floundering sites. It was December of 2013, and I realized that my trajectory would have me disabled in no time. So we began the paperwork, and then, seemingly out of nowhere, something extraordinary happened.
A new treatment came out, one with a 90%+ efficacy, Sovaldi. For the first time in my life, I had real hope. I pumped up my advocacy efforts and began writing for HepMag at the invitation of Lucinda Porter after she’d read my heart-wrenching story submission and subsequently my blog I’d started during my third treatment. The treatment had to be off-label and combined with another DAA called Olysio; the combo was the first treatment to bring me to a zero viral load. And not only that, it had almost no side effects; it was life-changing. My family and friends were excited for me, but this isn’t it. This isn’t the good part. It’s not even close. It was a high moment, where my family and friends enjoyed a month and a half of knowing I would live beyond thirty and maybe have a more typical life after I hit SVR12. These treatments all have a waiting period for when one can be cured. Because it takes time to know if the treatment has been effective. That date is called Sustained Viral Response at 12 weeks or SVR12. I never hit SVR12; in fact, not six weeks later, I was hospitalized for Clostridium difficile colitis (C.Diff.) The infection I’d acquired at a diner gave my remaining Hep C the chance it needed, my jaundice was so bad, my eyes were golden yellow, and I was bumped up on the transplant list. I spent the week at the hospital, wondering when and how I would leave. The idea of a transplant scared the hell out of me even though I knew it would ultimately save my life.
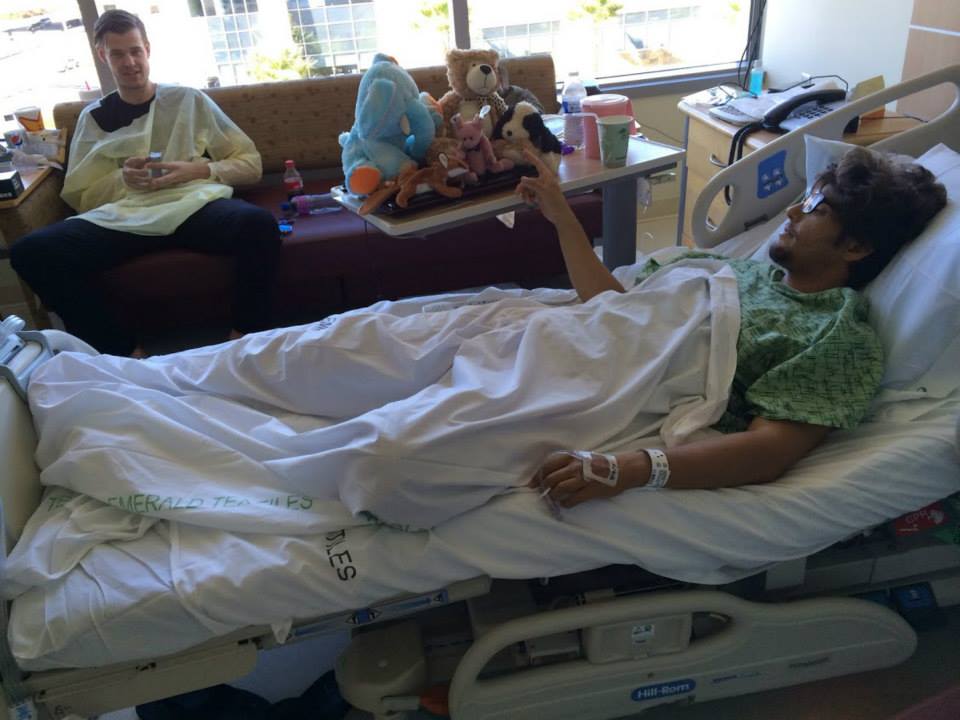
Two days in, they explained that my Hep C had returned. I wasn’t allowed to leave my room alone, but thankfully I had lots of friends and family come to visit. Even an old co-worker I hadn’t seen in almost two years heard about it and stopped by. Also, coming into the hospital with C.Diff is awful, but as I was spending a week there, at least I got my own room. I also wanted to confuse the CNAs, so I had everyone bring in stuffed animals and “congrats on your baby” things because humor is excellent medicine. Upon discharge, I was informed of a new treatment and was slotted to take it by the end of the next month in November. It had a higher success rate than my previous treatment at 98%; Harvoni also required 24 weeks due to the extent of damage done to my liver. But it was just as successful as the prior treatment; by six weeks, I’d hit zero, and I’d maintained it up until May. Then, as we prepped for the annual Liver Life Walk, I received the news that my last week on treatment, the virus had rebounded, and treatment failed again.
The walk was challenging, and my body started to have trouble dealing with the symptoms, even with the medication. The cascading failures put me into a deep depression, and my girlfriend-at-the-time felt equally depressed. Months afterward, our state degraded to an untenable point; the breakup, though, was fuel for change. Sometimes it takes a kick in the head to see a different perspective, to push someone out of a funk. I redoubled my efforts, crafted a routine to help me maintain my strength and fortitude, and told all of my friends to help watch for my HE symptoms, to tell me when I should take lactulose to help ease it. I jumped back into life and began searching to find out exactly why the treatments failed and see if any treatments could match my specific situation. I found the particular mutations and why my treatments didn’t work, so I proposed a combination of two treatments, combining Zepatier with Harvoni. My doc took it under advisement, but before anything could happen, my liver hit the point of no return. As my transplant doc described it best, my liver was an old shoe, and it needed to be replaced before I could go on another treatment. My three-year wait for a transplant had, so far, gone without a call for a full, healthy liver, so I knew it would be a challenge going forward. To keep my mental faculties and physical state intact, I followed a friend to dance class. There I found the perfect outlet to work around the temporary memory loss caused by HE by introducing muscle memory to my memory castle techniques for memorization. Dance was at my own pace. I kept a bag of intentionally chosen mixed nuts (the combo helped balance my electrolytes, which would constantly be a wreck because my body would purge the retaining fluid or expelling fluid from diuretics.) Dance gave me a lot of my world back, but as my jaundice became impossible to hide, sunglasses at night were harder to pull off. I started working with a newly formed coalition of nonprofits called CalHep and helped them pass a pilot program by speaking with the assembly subcommittee. I was committed to ensuring that no one else should go through the hell of end stage liver disease because it was unnecessary if they can get treatment. At that time, there were restrictions on access, so that you needed to be F3, which is when permanent liver damage begins, to start treatment. F3 is the third tier in the liver disease fibrosis scale; F4 is usually when MELD begins. While the F3 requirement is no longer the case in California, other states like Texas (at the time of this article’s writing, Dec. 2020) still have these heinous restrictions. As an advocate, I dedicated myself to helping in the fight to the best of my ability. But in September, I began a series of monthly hospital visits, which could eventually lead to my death or maybe a transplant, and everyone around me knew it. It was the most intense period in my life, and it also happened to be October of 2016.
So everything was becoming politically charged, and tribalism was making the fight for healthcare even harder. In September of 2016, I moved along with my friends from the apartments we’d lived in for three years into a four bedroom house. It was nice, and I’m thankful that my friends were able to do this with me, especially in the condition I was in. But in my shape, setting up for the move was hard, and during the process, I passed out while explaining, “no, I just need a double-double from In N Out.” What I didn’t realize is that the craving came from a complete lack of sodium in my body. In addition to that, I happened to be Hypocalcaemic, so when I arrived at the hospital, they quickly assessed the situation and were more surprised that I wasn’t in a coma, based on how low my sodium was. I spent the week in the hospital recovering while my friends packed up my remaining things and moved me into the house. When I got home, I started to organize my things and pack for a trip. My mom had decided that we should take a cruise ship to Mexico, so she invited me and even paid for a friend to come along. I understood why she was doing this, she wanted to have some good last memories if things should come to that, and she wanted me to have some enjoyment in this rather literal hell. But that’s not in keeping with the buzzard’s luck I seem to have.
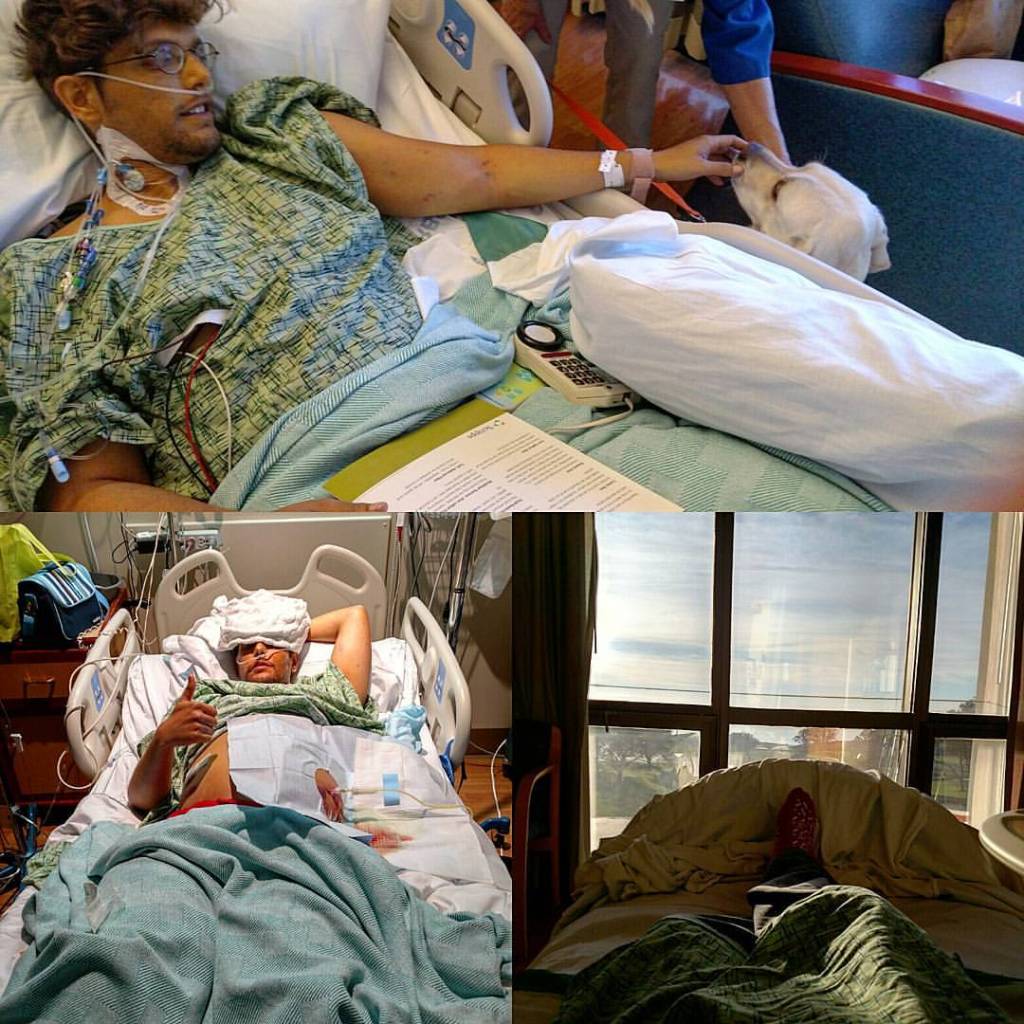
The trip was made more challenging by an odd bit of advice. Counter to literally every other doctor I’ve had, the attending doctor, during my last trip to the hospital, told me that to beat Hepatic Encephalopathy, I should really be consuming less protein and more salt. (just so we don’t spread this around, that’s TERRIBLE ADVICE, it’s the exact opposite of what should be done, low salt, high protein is correct.) But the thing is, when you have HE, memory is a tricky and confusing thing, so I followed his advice for a few weeks, including this trip. Needless to say, I looked straight up pregnant, my ascites were such that my stomach actually started to hurt on its own, and I spent most of the trip vomiting and walking in circles to avoid leg cramps because I didn’t pack my mixed nuts combo. When we returned from the trip, I found myself in so much pain, I couldn’t bend down to put on socks. The trip to the hospital had become so routine, I prepped my doc en route and told her what was going on. She confirmed what I’d suspected, I’d need a peritoneal tap. A peritoneal tap is typically a needle in the abdomen which drains excess fluid. Thankfully they were ready for my arrival, and they rushed me into triage and started work right there and were concerned. The reason for the concern was that peritoneal fluid can become septic if left for too long. And the pain was indicative of just that: sepsis. My heart rate was such that the only pain med I could take was Ketamine. As they drained twelve pounds of fluid from me and placed an Internal Jugular port in my neck to administer antibiotics in an attempt to knock out the sepsis. I was lucky that within 18 hours, the antibiotics were working, and I could slowly get better. This event had also raised my MELD from 26 to 35. I remember sharing my journey with every doctor who came in, explaining that should I live, I would get an Master’s in Public Health so that I might do more for my community. I shared my journey for two reasons, to remind myself of my purpose and to curb stigma. My higher MELD meant it was more likely that I could get a transplant, but I would wait and be denied not one but three potential transplants while the election day would frustrate my television set in the background.
Going home with a PICC line in, I didn’t know how long I’d have left; I felt better, but I knew it was relative. A Peripherally inserted central catheter line is a soft tube that goes in the left arm, allowing drugs to be more easily administered to the heart. I’d accepted and come to terms with my death should it come to that. I dug hard into my routine and got back to focusing on surviving, and waiting. I had had over eight viable liver offers at this point, and each time, renewed life was given to another person higher on the list than I. When you get to where I had, being called in for a liver offer is a regular occurrence, actually being the recipient however, is quite rare. The reason this happens is to make sure the liver goes to the person of most need where the liver and recipient will have the highest chance of survivability, they prep the top few contenders for transplant for every newly available liver.
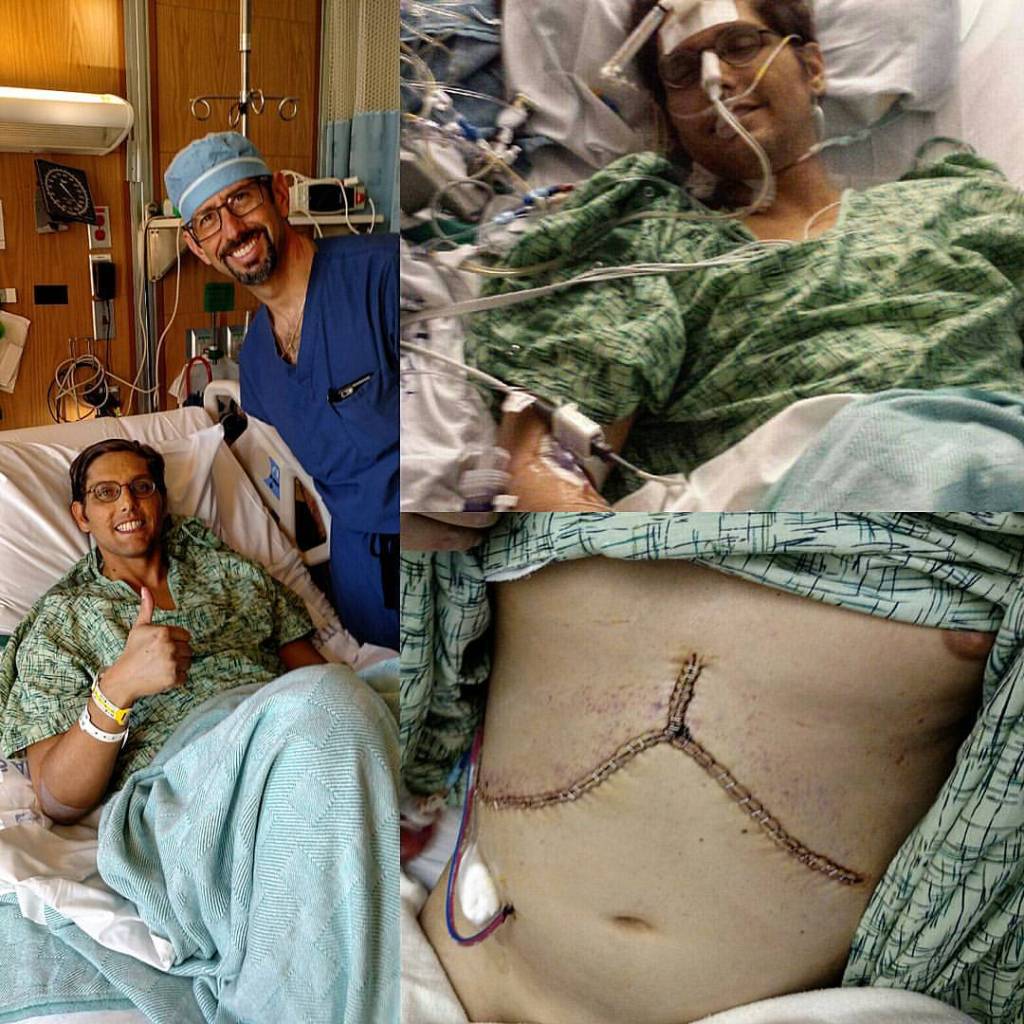
About three weeks later, on December third, 2016, I received the call for my transplant. That day is one of the most vivid blurs because only shortly after I arrived and cleaned up, I was prepped for transplant and put under. Five hours later, I was out. Everything had gone right, and within two days, I was farting! Okay, yeah, I get it, it doesn’t sound impressive, but it’s the first step in knowing that everything is hooked up and working correctly.
Within three days, I was out of the hospital and kinda walking, I had to do a rollout method to get out of bed, because well, my abs were cut in half, but one adjusts. I was back on the elliptical within the week and ready to get back into life. My friends and family all wanted to visit, but everyone had to wear masks and gloves because of my fragile immune state, and no one who was sick could come over. Once ready, I returned home and prepped for the next step in my recovery: treatment, again. Because if this treatment didn’t work, the virus would infect my new liver, and I would be reliving the last three years of my life as my new liver slowly failed. But thankfully, my doc expanded on what I’d suggested a year earlier, prescribing me twelve weeks of Zepatier, Sovaldi, and Ribavirin. An off-label treatment was designed to target my specific variant strain of HCV. It was approved by insurance (every previous medication had been denied and required multiple appeals to push through, but this one was on Medicare.)
It, too, had its bumps as insurance goes, as I didn’t zero out until eight weeks. My team was concerned I might not reach SVR24 because four weeks isn’t a lot of time to stay a zero viral load while on treatment when you have the history I do. After weeks of stressing, calling lawyers’ offices, and preparing for a large lawsuit should it need be done, I was relieved to get to SVR12, I wasn’t quite cured, but it was a good sign. Then, 18 years after my initial diagnosis, I was cured of HCV; in early September of 2017, I reached SVR24.
In 2017 I was already writing for HepatitisC.net, working with CalHep, the American Liver Foundation, and HepMag.com, but I needed to do more. In 2018 I started working with Help4Hep as a Peer Counselor; I stepped up at HepatitisC.net as a moderator. I stepped up my volunteering, speaking with ALF and Lifesharing, doing TV interviews to promote organ donation. Assisting CalHep in attempting to expand the pilot program I’d helped promote in 2016, and at the close of 2018, I was offered to be the Chair of the Consumer Committee at Eliminate Hep C San Diego. In 2019, I advocated with End The Epidemics and helped secure funding for HCV, HIV, and STD programs in California; I also started with a brand new nonprofit. Having been a patient advocate and a part of NoHep 2030 since it started, I knew that the goal is near impossible given our current prescription drug and healthcare system. This is why I started working for this new nonprofit, Open Biopharma Research and Training Institute. I realize that the prescription drug marketplace has many holes that increase prices, and one of those holes is manufacturing training, as there are drug shortages and lost development costs. So in an attempt to help smooth that process, I jumped at the chance to join Open Biopharma as the Director of Education and Outreach.
While preparing for the nonprofit’s launch, I finally began my Master’s in Public Health program on my third attempted application. I dove right in, researching and doing my first literature review on young people with Hep C. That Literature Review helped me craft an article that informed and encouraged others to comment on the new CDC recommendations for Hepatitis C testing. Every aspect of the new recommendations was adopted, and additional guidance reflected the research recommendations in my article. Additionally, End Hep C SD was officially kicked off in a unanimous vote by the San Diego County. It was terrific seeing advocacy work pay off, but by thesis working with HCV was muted by the arrival of COVID19. The project I’d intended on working with could no longer happen, so I dove into research on COVID19 and have since begun a systematic literature review as I am now in my final semester of my Masters’ In Public Health Program. Over the summer, I helped design health promotional material explaining the different SARS-CoV-2 antibody tests. Splitting my advocacy focus between COVID19 and Hepatitis C has been necessary. Those who are newly infected with COVID19, and COVID Long haulers, are not alone in their plight, and those of us in the HCV and HIV/AIDS communities who understand their fight have stepped up as well, like with COVIDhealth.com. We’ve already shown that when we fight to end multiple epidemics, we can sync up those fights. I look forward to graduating with my MPH in 2021 and publishing my journey with help from friends and family as a book in 2022.
Each year I plan on updating my story to share as the journey continues. If anything, I hope my story inspires you to help someone close to you who has Hep C, who you may not have understood the potential for their plight, or to help yourself remind you that you have so much more potential than you know. We are all worthy of treatment, care, and love. The more we share our stories, the more we can help erase stigma.
TLDR; When it comes to Hep C: Get Tested, Get Treated, Get Cured.
Senator Wiener Introduces Legislation to Establish a Master Plan to End the Epidemics of HIV, Hepatitis C and Other STDs
SB 859 would create a master plan requiring state agencies to set targets to end outbreaks of HIV, Hepatitis C, and other STDs
SACRAMENTO – Senator Scott Wiener (D- San Francisco) introduced a bill today that would require state agencies to establish and implement a master plan to end new infections of human immunodeficiency virus (HIV), hepatitis C virus (HCV), and other sexually transmitted diseases (STDs). The diseases disproportionately impact gay and bisexual men, African American men, and young people ages 15-24. Though many effective preventative and treatment tools exist today, these epidemics still persist. In a society where we have the ability to treat and prevent against new infections, it is unacceptable that the rates of infection have barely slowed, and have increased in communities of color.
From 2013-2017, new HIV diagnoses decreased 2% in the African American community and increased by 4% in the Latinx community, while declining nearly 13% among white people. And, comparatively, in New York, since the implementation of a master plan to end new HIV infections in 2014, diagnoses are down 40%. California’s preventative work is falling dramatically behind other states, and it is time to take a more thorough approach to ending these epidemics.
Senate Bill 859 would require the Secretary of California Health and Human Services (HHS), in coordination with the Chief of the Office of AIDS (OA), to create a comprehensive Master Plan to end new infections of HIV, HCV and other STDs. This bill mandates that the Secretary and Chief institute a Stakeholder Advisory Committee and work with relevant state agencies to set targets to end new infections and identify recommended programs, policies, strategies, and funding for achieving these targets.
Senator Wiener, the bill’s author and longtime LGBTQ rights activist who was the first elected official in the United States to openly discuss his use of PrEP, a preventative HIV treatment, said the following:
“We have the tools to end new infections of HIV and STDs. What we’re missing is political will. This bill, SB 859, would require California to make a plan to end this epidemic, and help state agencies access the necessary resources to do so. I’m proud to be introducing another piece of legislation fighting for the LGBT community, which, alongside other marginalized communities, is disproportionately impacted by HIV and other STDs. California must be a leader on these issues, and right now we’re at risk of falling behind. SB 859 would a big step towards finally ending the epidemic.”
“We have come so far in how we can diagnose, treat, and in some cases cure these diseases. They no longer have to be epidemics,” said Assemblymember Todd Gloria (D-San Diego), principal co-author of the legislation. “It’s time for California to lead and demonstrate that ending the HIV, HCV, and STD epidemics is possible. Creating a master plan to bring focus and collaboration to end these diseases is in the best interest of public health, taxpayers, and our future generations.”
“Creating a Master Plan on HIV, HCV, and STDs will address widening disparities among vulnerable populations and build upon the successes of the last 30 years,” said Assemblymember David Chiu (D-San Francisco). “I am proud to join Senator Wiener’s effort to bring California’s efforts to end these epidemics in line with other states.”
“STD rates in California have reached record highs and HIV and hepatitis C continue to impact the state’s most vulnerable and underserved communities,” said Craig E. Thompson, CEO of APLA Health. “We applaud Senator Wiener for leading this bold effort to bring together state agencies and community members to develop an aggressive strategy to end these epidemics. Now we need the full support of the Governor and the Legislature. The longer they wait, the more it will cost California to treat new infections that could – and should – have been prevented in the first place.”
“California can no longer respond to its HIV, HCV, and STD epidemics as if they are distinct public health crises. These epidemics stem from the same root causes: lack of access to health care and prevention services, stigma and institutional bias, and an insufficient, fragmented response from our public health system,” said Joe Hollendoner, CEO of San Francisco AIDS Foundation. “We are thankful to Senator Wiener for his leadership in calling for a statewide masterplan to end the epidemics and look forward to working together toward a future of health justice for all Californians.”
“Collaborative and concrete action to address skyrocketing STD rates is long overdue,” said Julie Rabinovitz, President and CEO of Essential Access Health. “A public health crisis of this magnitude requires a comprehensive statewide strategy to strengthen our public health infrastructure, increase public awareness about the importance of STD prevention, and expand access to STD testing and treatment for all Californians. We thank Senator Wiener for his leadership in calling for the development of a coordinated state work plan to end the HIV, Hep C, and STD epidemics in our state, and look forward to advancing this important measure this session.”
“San Francisco has long been a global leader in working to end new HIV infections, and just last year new HIV infections dropped below 200 for the first time ever,” said San Francisco Mayor London N. Breed. “We are, however, facing some of the same challenges that we see statewide, including reaching our Black and Latino populations and reducing new infections for people who are experiencing homelessness. We need the State to develop a comprehensive plan that will help our City, our region, and our State end the epidemic once and for all, and I thank Senator Wiener for his leadership on this important issue.”
SB 859 is sponsored by the SF AIDS Foundation and APLA Health and co-sponsored by Essential Access Health. Assemblymembers Todd Gloria and David Chiu are principal co-authors. Additionally, Senator Melissa Hurtado (D- Fresno) and Assemblymember Rob Bonta (D-Oakland) and are co-authors of the bill.
PLEASE COMMENT
The CDC has an open comment period until Dec 27, 2019.
Please follow the link below and support universal screening enhancement, and the ADDITION of re screening for high-risk groups, mirroring HIV testing
https://www.cdc.gov/hepatitis/policy/ScreeningComments.htm?fbclid=IwAR1xFq79XC3dUTnwo0LifIvTyWFUUsOVwevYDQlLJqWtTddRmqL8oJB5QPI
This isn’t an interview: Me to me.
(for those of you who would like to listen, rather than read, or just do both, I’ve recorded a reading of this entry )
My name is Rick Nash, just a few days ago i turned 31.
This birthday is special to me.
Because it is one I didn’t expect to necessarily have.
When I was in summer of my seventh grade year, I was diagnosed with Hepatitis C ( HCV.) One of the key elements I took from that doctor’s appointment was that I would need a transplant around 30, or die. And given the knowledge he had and the virility of my, to be later understood as, variant strain, a transplant would only extend my life a short period of time.
It was a prediction that I have fought against my entire life. Two months ago, I received a liver transplant. And presently I am on treatment for HCV, my viral load fell from 100 million to 33,000 at present following four days of treatment.
I am by not yet out of the woods, but I’m better off than he predicted. Because he also believed that my state would be far more impacted by the virus.
I stay healthy otherwise, and a life of keeping myself that way has helped me survive. But by no means could I be writing this now without the support of others near and far.
So this isn’t an interview, it’s just a format to help isolate certain issues, but what are we talking about?
Presently we are in dire straits politically, and many don’t understand just what the stakes are.
I’m talking about the ACA aka Obamacare.
First off, I want you to know that I am biased. After all without the ACA, I wouldn’t be here. To make this more complicated I’m going to now remind you that I’m a registered Republican, always have been. In fact, I come from a line of Republicans, my family has been here since Coolidge and I take pride in this.
So we’re essentially talking about how the ACA/Obamacare saved my life.
You’ve had a prexisting condition your entire life, one that insurance companies actively prefer to deny treatment for, how has that impacted your life?
I’ve been aware of healthcare and health insurance since high school. I learned how to understand benefits from my mom, who has worked in HR for as long as I’ve been alive. My senior year in college I began looking for a job that would give me the benefits I needed. I focused more on benefits packages than compensation, because of the high costs I would pay otherwise.
My first failed treatment in 2008 showed me the price to lose insurance. That treatment would have cost me over $60,000 even having failed and stopped halfway through. I graduated in 2008, and like many others at the start of the recession, finding any decent paying job was a challenge.
When I graduated I realized that I would need to stay in school full-time until I could get a full time job with benefits. So I enrolled in classes and worked 25-39 hours per week. When I found an available promotion, I seized it. I took a chance and began a second treatment, and while I was working 39 hours a week; making a living wage, in order to have benefits, I still went to school full-time.
I was lucky in that four months before I turned 25( my parents’ insurance had a policy that allows students under 25 to be on their parents’ plan) I managed to find a job with benefits.
That next year in 2011, I planned on starting treatment. With a solid job I could try the one that would eventually cure my mom. But a week before an esophageal bleeding episode would send me into the hospital, I was pink slipped. To make this more confusing, it would be recalled, and sent again twice.
After receiving my MELD Score of 14, I began to look for a new job. Thankfully my friends knew of an opening and I started later that year.
There was one problem. The company used a temp service to hire it’s own employees allowing them to bypass benefits, and their internal employee guidelines. Using a temp agency like this is common, and lives in a legal gray zone. The temp agency can’t exclusively cater to one company and/or be owned by the company.
Thankfully the ACA stepped in twofold: it extended my coverage until 26, and my preexisting condition was no longer a coverage concern.
That being said, the ACA was new and still very shaky, and insurance companies can retroactively deny coverage.
So I prepared myself for a potential situation wherein the ACA is repealed and my insurance retroactively kicks me off of it, using my preexisting condition as a cause.
What this meant for me is that I would need to use COBRA to extend coverage until I would start my new insurance in April. So for two months I would see nine hundred dollars a month fade away into nothing to insure my insurance would still carry me.
What would have happened without the ACA?
Without the ACA I would presently still be in debt from a six month coverage gap. Because as I would begin my new job, my left femur was injured in a car accident. While her insurance covered the losses, it was reimbursed months after the collision. I would not have been able to cover my medical bills, or any other incidentals. My HCV treatment without insurance was over $100,000 and the medical care otherwise meant I hit max out of pocket on a yearly basis.
Meaning I would have no choice but accumulate unpayable amounts of debt with the hope that bankruptcy could possibly save me. Which would limit my housing options, my ability to cover future medical costs, and any potential use of my economics degree.
Thankfully, the ACA does exist, so that didn’t happen.
Those two parts of the ACA/Obamacare legislation were vital in your life, how else has it affected you?
After the third treatment failed at the end of 2012, my symptoms began to worsen.
Ascites, an extreme form of water retention, became an issue of vigilance. While I was prescribed a solution in the form of diuretics, I would only need to take them occasionally. Because if I failed to, and kept to them, my legs would randomly spasm out of control.
I would find a method that would keep me moving and alleviate the issue: Balancing my electrolytes. While I couldn’t control how my liver used them, I could make sure I was always consuming a specific amount.
The ACA required restaurants of a certain size to post nutritional information, and increased requirements on packaged foods. Without that, it would have been incredibly challenging to navigate.
The amount of magnesium, sodium, potassium sugar and water would change, and I learned how to understand each different pain and what it associated with. It took months to find that balance. Unfortunately, I was terminated at the end of 2013. While the termination was unlawful and discriminatory, fighting it wasn’t an option. While I was legally disabled, disability would take time and would not be enough to cover the cost of health insurance. While it did allow MediCal/Medicaid, my treatment wouldn’t have been covered under it at that time. So I worked as much as i could, enough to obtain insurance.
Wait, you were legally disabled, why didn’t you have disability Medicare?
When you become disabled, it can take between two and three years until you can have access to Disability Medicare. I guess they hope that you die before you need it. Because, of all the laws and decisions I’ve read, I can’t figure what their rationale is.
Without a job I was frantically familiarizing myself with Covered California.
Covered California is the California specific version of Healthcare.Gov the ACA marketplace, there are a lot of mixed feelings about its pricing, where do you stand?
First off, the marketplace prices are set by private insurance companies. And because of this marketplace smaller locally based hospital-insurance hybrids have been growing. The prices are still primarily controlled by two elements: the top four insurers, and the banks that are invested in these insurance companies.
Sounds like you’re into conspiracy theories.
Technically, that’s what this is, they’re conspiring to control prices. We have no way to correct this market inequality besides government action.
The ACA allowed me not only access, but because my income was eligible for the credit, I was able to purchase an affordable plan and keep my doctor.
It allowed me to postpone my death by a year as I zeroed out on my fourth treatment. The victory was short lived as I hit my out of pocket maximum, a four thousand dollar deductible and a week in the hospital after a run in with C.Diff at a diner. The treatment had failed and the virus was back in the millions.
Thankfully I soon began a fifth treatment. The year ended and new insurance plans came up, the one I was on previously was shuffled a bit so they could legally increase the price.
The plan increased in price by about forty dollars per month, a 13% increase with few noticeable changes in benefits. While irritating and burdensome, it was still far better than the alternative. Each of these treatments combined cost me out of pocket only about $12,000. Which may sound absurd for an income of $18,000 per year but remember that without it, if I could even get the treatment, I would be out over $300,000 on treatments alone.
To date my cumulative bill to insurance total is approaching six million dollars.
TIL: I’m not a cheap date.
It was worth it though, you were cured right?
No, the fifth treatment failed, and within a year my liver went from an average MELD of 20 to 30. I was steadily dying, and it was visible. To hide the jaundice I maintained a tan; however, by June the jaundice made me look more orange than anything else.
My treatment was postponed as I was no longer allowed treatment due to my high MELD score, and so I waited by my phone. I had been on the transplant list nearly three years by this point and only received two calls before September of last year.
Before I would be between hospitalizations near the end of the year, my Disability Medicare finally came in. While it is more expensive per month than my previous plan, I was able to have three weeks of hospital stays, a week of at home nursing, and dozens of RXs taken care of for very manageable copays… Oh and a liver transplant and subsequent medication.
It sounds like the ACA was the bridge before Medicare for you, was that always the plan?
No, no one means to be sick, I did everything in my power to live and utilize the tools I had access to. I didn’t want to get to the point where I needed Medicare. But I can say this comparatively, having it is one of the most relieving insurance plans I’ve had.
So you’re alive today because of the ACA and Medicare, how do you feel about the repeal and replace?
I’m interested to watch as the GOP replaces The ACA/Obamacare with The ACA/Obamacare or Ryancare.
Don’t you mean Trumpcare?
No, Trump has nothing to do with helping anyone but himself, while I disagree with Paul D Ryan on most things, he is the congressman who will craft a replacement. He has been at the head of this opposition since the ACA came into being.
https://krugman.blogs.nytimes.com/2011/06/03/ryancare-versus-obamacare/?_r=0
Like the Sanders v Cruz debate, the GOP wants to keep things vague, they don’t stand for anything until the day they vote. Unless they author/co-author legislation. It’s their M.O. because if you haven’t taken a stance, citizens are less likely to be angry with your decision.
We can change this, we can make sure we have a good healthcare system. Just call your local Congressperson and/or Senator and tell them what you like or don’t like about the ACA/Obamacare.
A legal document must be read through and through, to understand it’s gravity.
I say gravity because it doesn’t just affect its intended target, it affects everything around it. The ACA aka Obamacare is one of the most powerful pieces of legislation I have seen in my lifetime. It saves lives, improved lives, expanded Medicaid to millions and expanded potential millions in productivity while decreasing the reliance on (medical bill related) bankruptcy.
After all, a healthy workforce earns more, spends more, and lives longer.
New things to come.
I’m going to do something positively terrifying.
Come March 14th not only will I know what’s going on with the Zepatier Treatment
But across all of my online dating profiles I will openly disclose that I have HCV along with pertinent information.
My virtual identities which I once held separate I’m going to link.
I don’t really know what will happen.
I don’t know how people will take it.
But we’ve all got our shit.
In addition to doing the ongoing dating series…
Next month The Five will be available to read in it’s first iteration in six parts. 
It is an introspective look at the previous treatments’ failure and how to fail best.
(like Astronaut Chris Hadfield says “Visual Failings, not Defeat” )
Ch Ch Ch Changes
In the next few weeks HCVME.org will be re-vamping with some helpful healthcare guides.
In the meantime sit back, and enjoy my weird mixture of blogs and men. It’s my blog. It’s not about men, lets just be content with the content and read more into the context, so that it’s not conned text. Sometimes i’m awed by the odd. Perhaps my two cents would make more sense, if allowed to be read aloud.
But it’s perhaps you read what you read and most impotently you might be homophonic.